Initial Sjögren’s Symptoms May Predict Severity of Lung Complications, Study Suggests
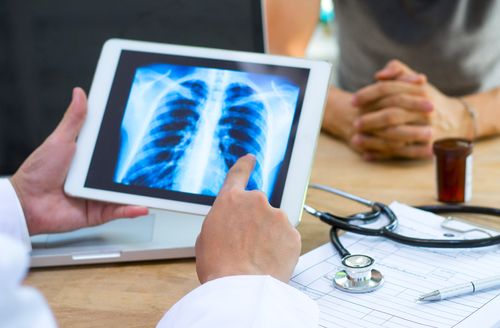
Patients with primary Sjögren’s syndrome whose first symptoms are not mouth and eye dryness may experience more progressive and severe pulmonary manifestations during the course of their disease, a study reports.
The study, “Interstitial lung disease in non-sicca onset primary Sjögren’s syndrome: a large-scale case-control study,” appeared in the International Journal of Rheumatic Diseases.
Sjögren’s syndrome is an autoimmune disease characterized by the infiltration of immune cells into secretory glands — primarily the lacrimal and salivary glands. These cells incorrectly recognize the glands’ tissue as foreign and fight it, leading to cell death and reduced production of tears and saliva, resulting in dry eyes and dry mouth, or sicca.
In some patients, however, the disease may have manifestations outside the secretory glands and cause systemic symptoms, including lung disease.
Lung symptoms appear in anywhere between 9 and 75 percent of Sjögren’s patients, depending on the diagnostic tests used.
Because systemic symptoms are the main determinants of a patient’s prognosis, early detection and treatment of such complications are a major concern among physicians.
Researchers at the Peking University People’s Hospital in China set out to compare the frequency and severity of lung disease between patients with and without sicca at disease onset.
Among the 1,341 patients admitted to the hospital between 2003 and 2012, 853 had primary Sjögren’s syndrome and 488 had secondary Sjögren’s syndrome — meaning the disease was caused by another condition.
More patients with primary Sjögren’s had lung involvement than those with secondary disease — 25.8% versus 19.3%.
Investigators then examined the clinical records of 102 primary Sjögren’s syndrome patients, hospitalized between 2008 and 2012, and whose computed tomography scans were available for analysis. The majority of these patients were women (91.2 percent), with a mean age of 61 years.
Half of them experienced sicca as their first disease manifestation. The other half had pulmonary symptoms — such as shortness of breath or coughing — joint pain, fever, blood or vessel problems, teeth loss, rashes, parotid gland swelling, or liver damage.
While the mean time from the first symptom to diagnosis was similar, more patients with sicca were diagnosed with primary Sjögren’s syndrome at disease onset than those with other symptoms — 34% versus 4%.
Non-sicca patients required salivary gland biopsies or radiological examinations of the salivary glands more often than those with sicca at disease onset. They also required more lung biopsies and lavages.
Patients without initial sicca also had lower levels of globulin, a marker of liver function and inflammation, and anti-SSA and/or anti-SSB autoantibodies, as well as elevated rheumatoid factor.
Regarding pulmonary manifestations, interstitial pneumonia was more commonly seen in non-sicca patients. Their predicted total lung capacity and forced vital capacity — measures of lung function — were also lower than patients with initial sicca symptoms.
“Non-sicca is a common initial manifestation in primary Sjögren’s syndrome with ILD,” the researchers wrote. These patients are susceptible to “more progressive and severe” pulmonary complications than sicca patients.






